These Surgeries and Medical Procedures are Performed Too Much On Black Men – BlackDoctor
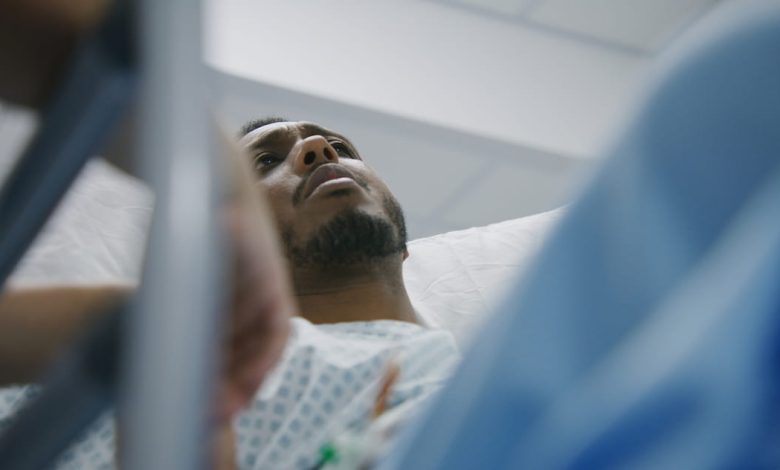
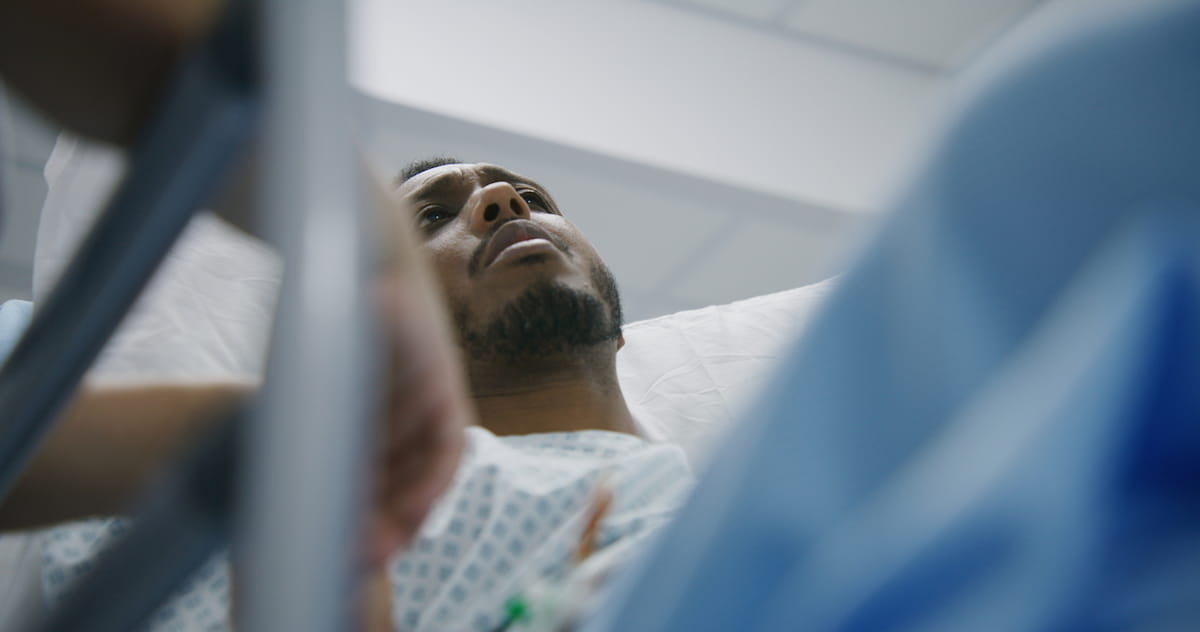
For decades, researchers have examined a critical question in American healthcare: Are Black men subjected to more surgeries or invasive medical procedures than other groups?
The answer is complicated. In some cases, Black men do undergo certain procedures at higher rates—particularly amputations, dialysis-related surgeries, and emergency interventions. But the underlying story is not simply over-treatment. Instead, it reveals a deeper issue: systemic inequities that lead to more severe disease and fewer preventive options.
This article breaks down the data, the patterns, and what’s really driving these disparities.
Before diving into specific procedures, it’s important to understand a key paradox:
- Black patients are often less likely to receive early or preventive care
- But more likely to require invasive procedures later
This pattern is widely documented across U.S. healthcare systems and reflects structural inequality, access issues, and bias rather than biology alone.
1. Amputations: One of the Starkest Disparities
One of the clearest examples of excessive procedures is lower-limb amputation.
Key Stats:
- Black patients are up to 3 times more likely to undergo amputations than other groups
- These amputations are often linked to complications from diabetes and vascular disease
Why this happens:
- Delayed diagnosis of Type 2 Diabetes
- Limited access to specialists (like vascular surgeons)
- Less access to early interventions that could save limbs
In many cases, amputations are preventable, making this one of the most troubling examples of disparity.
2. Prostate Cancer Surgery: More Aggressive Treatment
Black men face the highest prostate cancer burden in the U.S.
Key Stats:
- 1.4× more likely to be diagnosed
- 2–3× more likely to die from prostate cancer compared to white men
What this means for surgery:
- More likely to need aggressive treatment, including surgery
- More likely to be diagnosed at advanced stages, limiting less-invasive options
At the same time:
- Black men are often less likely to receive early screening tools like MRI (nearly 44% less likely after abnormal tests)
Result: More invasive procedures later, when the disease is harder to treat.
3. Dialysis & Kidney Procedures: A Lifetime of Intervention
Black men are disproportionately affected by end-stage kidney disease, requiring ongoing medical procedures.
What the data shows:
- Higher rates of dialysis and related surgical access procedures
- Higher hospitalization and mortality rates even when receiving treatment
Dialysis itself is not a one-time procedure—it often requires:
- Surgical creation of access points (fistulas or grafts)
- Repeated interventions over time
This leads to more frequent and ongoing invasive care compared to other populations.
4. Emergency Surgeries vs. Preventive Care
Another key disparity is how and when surgeries occur.
Research shows:
- Black patients are more likely to receive surgery in emergency settings rather than planned care
- In segregated healthcare systems, Black patients were 41–96% more likely to undergo surgery at lower-quality hospitals
This suggests:
- Conditions are often more advanced by the time treatment happens
- Surgeries are performed under riskier, less controlled conditions
5. The Hidden Reality: Some Surgeries Are Also Underused
While some procedures occur more often, others are underutilized in Black men:
- Nearly 40% less likely to receive certain prostate-related surgeries for non-cancer conditions
- Less likely to receive cardiac procedures or referrals despite higher heart disease risk
This creates a dual problem:
- Overuse of emergency or late-stage procedures
- Underuse of early, preventive, or elective care
The data consistently points to several root causes:
1. Structural Inequality
- Unequal access to insurance, specialists, and quality hospitals
- Healthcare systems serving Black communities often under-resourced
2. Delayed Diagnosis
- Less access to screenings → disease progresses further
3. Implicit Bias in Healthcare
- Differences in how symptoms are interpreted and treated
- Fewer treatment options presented to Black patients
4. Socioeconomic Barriers
- Transportation, cost, and time constraints delay care
5. Medical Mistrust
- Rooted in historical and ongoing inequities in care delivery
The evidence shows that Black men are not simply “over-treated.” Instead, they are:
- More likely to experience advanced disease
- More likely to require invasive, high-risk procedures
- Less likely to receive early, preventive care that could avoid surgery altogether
In many cases, the higher rates of procedures reflect a system where intervention comes too late.
The Real Solution
Reducing these disparities will require:
- Earlier and more equitable screening
- Improved access to preventive care
- Addressing bias within clinical decision-making
- Investment in healthcare systems serving Black communities